Faecal incontinence may be due to central or peripheral causes. Peripheral causes include those due to a weak pelvic floor, a weak or injured anal sphincter or impaired nerve supply to the sphincter (pudendal neuropathy). These all require investigation, with significant improvement in continence frequently achieved with a combination of biofeedback, medical management and surgery.
Cause
Weakness of the pelvic floor and anal sphincter and pudendal neuropathy all occur with age and with the hormonal changes associated with post-menopause. Multiple vaginal deliveries or a difficult prolonged labour increase the risk of both pelvic floor and anal sphincter weakness.
Symptoms
Faecal incontinence may be complete or incomplete. “Complete incontinence” implies incontinence all the time to flatus, liquid and solid stools. “Incomplete incontinence” implies that continence is sometimes achieved. It may be that incontinence is only with liquid or flatus, or that incontinence occurs only when away from nearby toilets, or occurs only at particular times (e.g. during coughing, straining or exercise).
Investigations
Your Colorectal Surgeon can organise anal physiology testing, which include the following:
- Endo-anal ultrasound (looking for defects in the anal sphincters)
- Anal manometry (measuring resting and squeeze pressures)
- Pedundal Nerve Terminal Motor Latency Testing (to exclude a pudendal neuropathy)
Course
Incontinence is usually slowly progressive and therefore should be treated early.
Medical management
Improved stool consistency, with bulking agents with non-absorbable cellulose such as psyllium husk (Metamucil®) or ispaghula husk (Fibogel®) or firming agents including loperamide (Gastrostop®) or atropine sulfate (Loperamide®) may improve continence.
Biofeedback
Biofeedback has been shown to improve incontinence. Those with complete incontinence with inability to raise their squeeze pressure on manometric testing are unlikely to benefit. These exercises can by taught to you by our practice nurse consultant.
Colonic lavage
Colonic lavage with enemas can ensure an empty colon prior to anticipated activities where an episode of incontinence may be inconvenient. A Fleet® enema, gently inserted into the anus, and retained for 15-20 minutes, can successfully empty most of the colon. A second enema may be needed shortly after the first if there are difficulties holding onto the first enema for the full 15-20 minutes.
Surgical management
Those with regular incontinence episodes and those whose lifestyle is severely affected by incontinence have the most to gain from surgery.
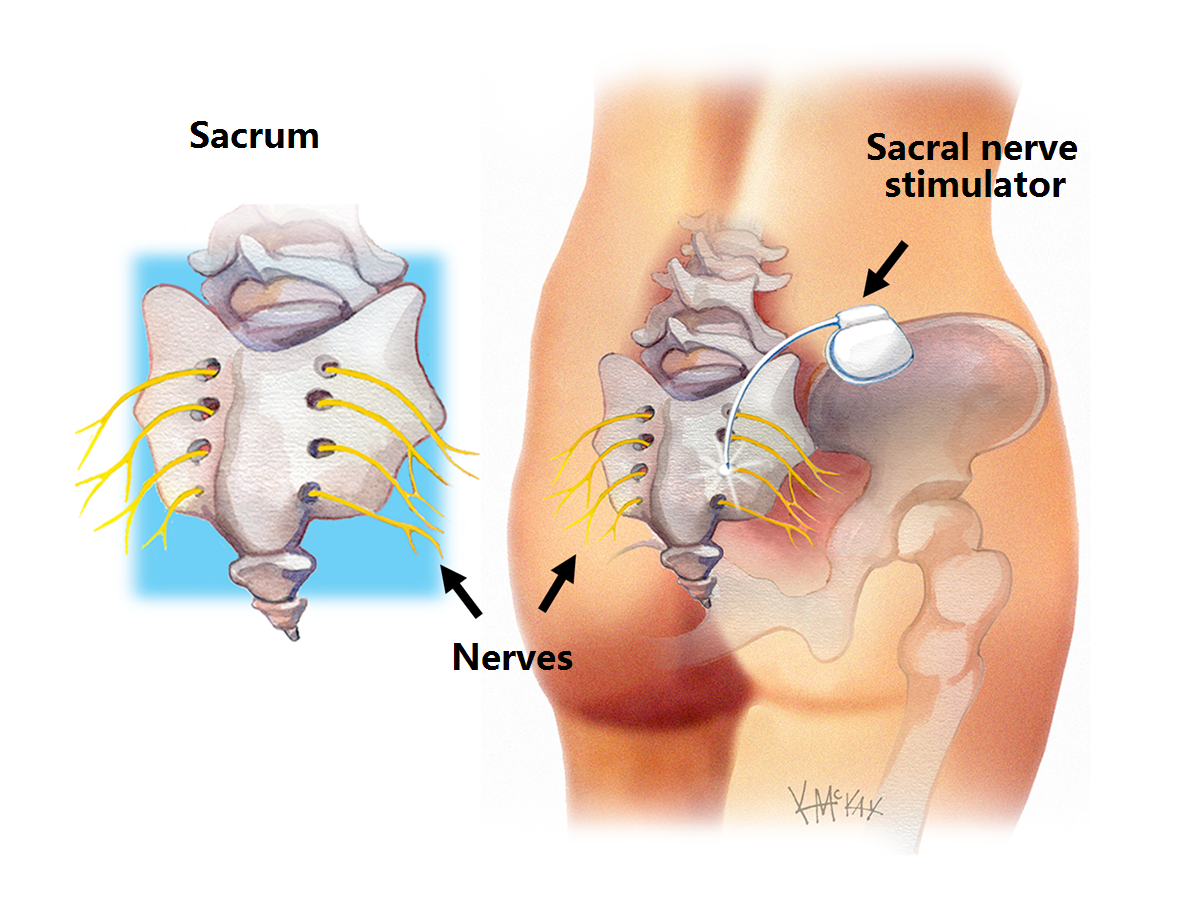
Surgical options include those to repair the anal sphincter (Anterior Overlapping Sphincter Repair) the pelvic floor with restoration of the acute rectosigmoid angle (Postanal Repair), or to reinforce the anal sphincter (Dynamic Gracilloplasty), or those that stimulate the pudendal nerve that supplies the anal sphincter (Sacral Nerve Stimulation).
Injectable Bulking Agents include products such as silicone (PTQ®) or pyrolytic carbon-coated beads (Duraspheres®). These can be injected to add bulk to the thinned or stretched anal sphincter. Injection of such agents is relatively safe and non-invasive, however the long –term benefits are only marginal.
Bringing out a stoma to divert faeces either with a colostomy or an ileostomy is rarely performed generally a last resort for severe faecal incontinence or where other methods have failed. In most cases this can be performed laparoscopically avoiding an incision.
What to expect pre and post operatively for faecal incontinence surgery?
Unless you are also having a colonoscopy, a normal diet without a bowel prep is required the day before surgery. You need to fast from midnight the night before if your surgery is scheduled for the morning, or from 6am if scheduled for the afternoon. You will be admitted as a day-stay procedure. You will receive a Sodium Phosphate (Fleet®) enema 1 hour prior to your operation. Immediately after your procedure you can eat a normal diet, but should have fibre such as a tablespoon of psyllium husk (Metamucil® or Fibogel®) twice a day. Occasionally a stool softener such as lactulose (Duphulac®) or sterculia (Normacol®) is also required. If you have had a perianal procedure, then twice daily warm salt water (sitz) baths are antiseptic to the area and encourage healing. If you have had a sacral nerve stimulator, you must keep the dressings intact and may shower but not bath for 1 week following the procedure.