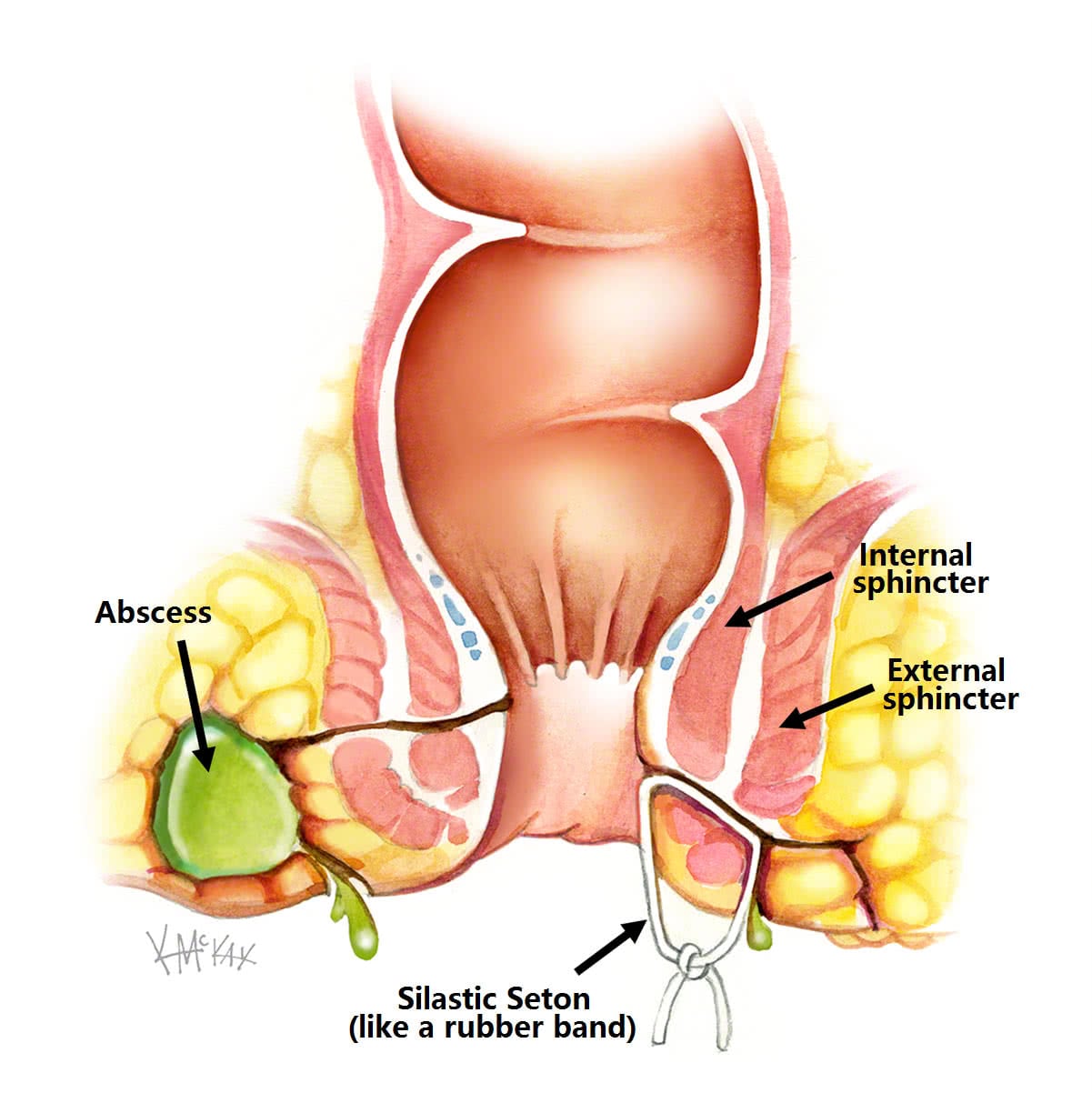
The initial management of a fistula is to drain it. This is a small surgical procedure performed under general anaesthetic where a silastic seton (similar in size and consistency to a rubber band) is passed through the fistula tract and tied in place. This allows any pus to drain, and inflammation to settle (figure 1).
A course of antibiotics may also be required. Within 6 weeks, the condition should be much improved, and you will need to be re-examined by a colorectal surgeon. There are 5 options at this point which include:
- remove the seton and hope that it heals
- leave the seton in place awhile longer or indefinitely with or without periodic tightening;
- remove the seton and lay open the tract cutting the muscle;
- remove the seton and remove the fistula tract with or without a flap repair; or
- remove the seton and use glue or a plug to seal the tract.
Remove the seton and hope that it heals
If the seton has been in for up to 6 weeks, and the infection has settled, some advocate simply removing the seton with success rates reported in up to 75-80% of cases[3,4]. This is best done before 6 weeks, as waiting longer than this can result in the formation of skin (epithelium) within the fistulous tract which can prevent its spontaneous closure. Caution should be taken in those with Crohn’s disease, where recurrence rates are very high with this technique[5].
Leave the seton in place awhile longer or indefinitely with or without periodic tightening
If the fistula tract involves a significant proportion of the anal sphincter muscle, it may not be safe to lay open the fistula tract, as that would involve cutting too much of the anal sphincter muscle, and this could potentially result in some degree of faecal incontinence. Therefore, the seton may be left in place awhile longer or even indefinitely. This ensures further drainage of any abscess and settling of inflammation. Sometimes a loose seton is re-tightened until it is snug with the aim of slowly cutting through the anal sphincter muscle (tight cutting seton). With repeated tightening, the seton slowly lays open the fistula tract, with the seton eventually falling out on its own without need for incising the anal sphincter. This slow process can take up to a year.
Occasionally, the seton eventually works its way out without the need for tightening (loose cutting seton), with the seton slowly cutting through the anal sphincter muscle. However, this can take years, but is safer than a tight cutting seton, as the sphincter has time to heal and repair itself as the fistula tract is slowly laid open[6].
Remove the seton and lay open the tract cutting the muscle
If the seton involves less than a third of the internal anal sphincter muscle, then it may be reasonable to remove the seton by laying open the fistula tract and cutting the overlying muscles. This allows cleaning (curetting) of the fistula tract, to promote its healing. Examination with endoanal ultrasound, and probing with Lockhart Nummery probe is necessary prior to this procedure to ensure that less than 30% of the internal muscles sphincter is involved.
Remove the seton and remove the fistula tract with or without a flap
If the seton involves a large amount of anal sphincter, the seton may be removed, and a formal excision of the fistula tract performed. This is an operation best performed after 12 weeks (or even longer), to allow complete resolution of sepsis and the formation of a definite epithelial-line or fibrous fistula tract that is well defined and therefore easier to surgically remove.
This may involve simple ligation and excision of a portion of the fistula tract, without the use of a flap (i.e. LIFT procedure) or may involve excision of the entire length of fistula tract followed by a formal flap repair to cover the internal opening.
If the internal opening is high in the anal canal a rectal advancement flap is performed using a flap of mucosa and the underlying muscle to cover the internal opening. If the internal opening is low in the anal canal, an anoderm V-Y advancement flap may be preferable. Both these flap repairs also involve repairing the sphincter, and cleaning (curetting) the external opening to allow ongoing drainage until the repair has healed.
Remove the seton and use glue or a plug to seal the tract
A vast number of plugs and glues have been used to try to seal fistula tracts. The benefit of these techniques is that they preserve the anal sphincters.
Initial results with fibrin glue were promising. Several products are commercially available and treatment involves single or repeated injection into the external opening. Initial studies were promising with healing rates of up to 70% with no studies reporting impairment of continence. However more recent studies looking at long-term healing rates show disappointing recurrence rates as high as 75% [7]
The fistula plug is made of collagen. Initial results were encouraging with high success rates [8]. However, long-term results are disappointing, with failure rates as high as 70-80% [9-10]. Therefore, a selective approach is recommended, with only some fistulae suitable for plugs. There is some evidence suggesting that long tracts greater than 4cm in length are more likely than short tracts to heal with these techniques [11].
What to expect pre and post operatively following anal fistula surgery
Fasting and Bowel Preparation
Unless you are also having a colonoscopy, a normal diet without bowel preparation, is required the day before surgery. You need to fast from midnight the night before if your surgery is scheduled for the morning, or from 7am if scheduled for the afternoon. You will be admitted as a day-stay procedure. You will receive a fleet® enema 1 hour prior to your operation.
Recovery and transport
Following your procedure, you will recover for an hour until the effects of sedatives have worn off. You should not drive yourself home after your procedure and should have someone organised (a friend or relative) to accompany you.
Bleeding
Spotting of blood or persistent minor oozing will occur for 5 days following your procedure, and a sanitary napkin changed once to twice daily will be needed to prevent staining of your underwear. Bleeding will typically occur after opening your bowels. If the bleeding is more than a couple of teaspoons a day, notify your surgeon.
Laxatives
You should remain on regular laxatives and simple analgesics for 1 week. A tablespoon of natural psyllium husk (Metamucil® or Fibogel®) twice daily, and 30ml of lactulose (Duphalac®) once to twice daily is recommended.
Pain control
For pain, a non-steroidal is recommended such as 400mg of ibuprofen (Brufen®) along with 2 tablets of paracetamol. This should be taken regularly three times a day for five days. Opioid medications (Endone) may sometimes be needed, but should be used sparingly as they cause constipation.
Antibiotics
After discharge from hospital you may require antibiotics to treat ongoing infection. Oral cephazolon (Keflex®) and metronidazole (Flagyl®) may be needed for 5 days (provided no allergies exist).
Dressings
Occasionally you may be sent home for daily dressings for up to a week, which is often performed by a community nurse or your local general practitioner. A thin silastic Seton may be inserted into your anal fistula. This is about the size and consistency of a rubber band and is passed through the tract of the fistula to allow ongoing drainage of the abscess. It is typically tightened or removed at 6 weeks.
Sitz baths
Twice daily warm to hot salt water (Sitz) bathing to the anal region is soothing and antiseptic, and should be done for 1 week following your procedure. Put a handful of salt into a shallow bath of warm-to-hot water and sit there for 10-15 minutes.
Follow-up
You should follow up with your colorectal surgeon in 6 weeks following your surgery to review your wound and discuss further management if indicated.
References
- Williams JG, Farrands PA, Williams AB, Taylor BA, Lunniss PJ, Sagar PM, Varma JS, George BD. The Treatment of Anal Fistula: ACPGBI Position Statement. Colorectal Disease. 9 (Suppl. 4): 18-50, 2007.
- Sands B, Anderson F, Bernstein C, Chey W, Feagan B, Fedorak R, Kamm M, Korzenik J, Lashner B, Onken J, Rachmilewitz D, Rutgeerts P, Wild G, Wolf D, Marsters P, Travers S, Blank M, van Deventer S. Infliximab maintenance therapy for fistulizing Crohn’s disease. The New England Journal of Medicine New England Journal of Medicine. 350 (9): 876–85, 2004.
- Joy HA, Williams JG. The outcome of surgery for complex anal fistulas. Colorectal Disease. 4: 254-61, 2002.
- Eitan A, Koliada M, Bickel A, et al. The use of the loose seton technique as a definitive treatment for recurrent and persistent high trans-sphincteric anal fistulas: a long-term outcome. Journal of Gastrointestinal Surgery 2009; 13(6):1116-9.
- Faucheron JL, Saint-Marc O, Guibert L, et al. Long-term seton drainage for high anal fistulas in Crohn’s disease–a sphincter-saving operation? Diseases of the Colon & Rectum 1996; 39(2):208-11.
- Lentner A. Wienert V. Long-term, indwelling setons for low transsphincteric and intersphincteric anal fistulas. Experience with 108 cases. Diseases of the Colon & Rectum. 39(10):1097-101, 1996 Oct.
- Buchanan G, Bartram C, Phillips R, etal. The efficacy of fibrin sealant in the management of complex anal fistula: a prospective trial. Diseases of the Colon and Rectum. 46: 1167-74, 2003.
- Johnson E, Gaw J, Armstrong D. Efficacy of anal fistula plug vs. fibrin glue in closure of anorectal fistulas. Diseases of the Colon and Rectum 49(3): 371-6, 2006.
- van Koperen PJ. Bemelman WA. Gerhards MF. Janssen LW. van Tets WF. van Dalsen AD. Slors JF. The anal fistula plug treatment compared with the mucosal advancement flap for cryptoglandular high transsphincteric perianal fistula: a double-blinded multicenter randomized trial. Diseases of the Colon & Rectum. 54(4):387-93, 2011 Apr.
- Ortiz H, Marzo J, Ciga MA, Oteiza F, Armendariz P, de Miguel M. Randomized clinical trial of anal fistula plug versus endorectal advancement flap for the treatment of high cryptoglandular fistula in ano. Br J Surg. 2009;96:608–612.
- McGee MF. Champagne BJ. Stulberg JJ. Reynolds H. Marderstein E. Delaney CP. Tract length predicts successful closure with anal fistula plug in cryptoglandular fistulas. Diseases of the Colon & Rectum. 53(8):1116-20, 2010 Aug.